In complex system, even small changes can have big, unexpected consequences. These are occasionally beneficial but more often than not have a negative impact.
Over the last year we have started to see some evidence for unintended consequences from the health care reform act. Negative impacts that we see are of two kinds: Perverse effects that directly affect the objectives of the act and side-effects that manifest in seemingly unrelated areas (see figure below).
It is not the intent here to comment on the overall merits or demerits of health care reform, but merely to describe some of these emerging (and potential) negative unintended consequences.
Side-effects:
Much of the discussion on the impact on employment has focused on the high cost of insurance. That issue would have existed with or without reform. The real impact of reform on employment resides in its side-effects.
For instance, we have seen over this last year that specific industries hit by additional taxes or penalties in the act have started to shed jobs. Medical Devices companies, for one, faced with a 2.3% excise tax have laid-off hundreds of workers. Clearly the increased demand from having more people covered is not seen as a sufficient offset to the tax hit.
Other side effects will show up in the near future. For instance, some small employers will choose not to employ an additional person if doing so triggers a penalty for them. An employer with more than 50 full time employees faces severe penalties if even one employee receives premium subsidies, penalties to the tune of $40,000 or more. Noting that the subsidy threshold for a family is higher than that for individuals, a second order effect of this is that it in such situations losing your job will make it harder for your spouse to get a job. Similarly, as a consequence of a different clause, some small companies will manage to a 50 employee size and keep average wages below $50,000 in order to receive tax credits for providing coverage.
Finally, there will be what economists call “notch distortions” in wages because, at certain levels of compensation, receiving a small pay raise will push an individual out of a subsidy level and result in a net loss of income[1]. A one dollar raise that puts someone beyond a subsidy threshold can mean a several thousand dollar reduction in income so we’re going to see a downward pull on wages just below the income thresholds for different subsidy levels.
Perverse effects:
The reform act dramatically increases the number of people with coverage. Yet, since the act does not increase system capacity, and because of the social equalization built in, there are several perverse effects that negatively impact the very objectives of the act.
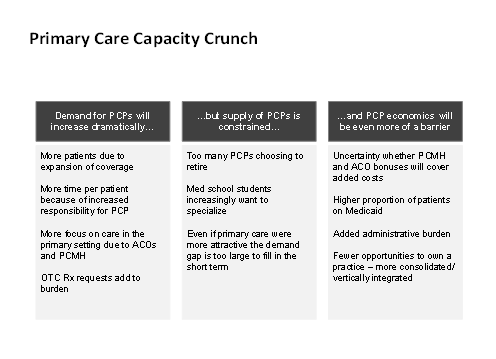
As is well-known, access to primary care is capacity constrained, in particular in rural areas and for Medicaid patients who are often unprofitable for providers[2]. In the short term, reform increases stress on primary care capacity. PCPs are expected to do much more in terms of covered preventive services, administration of Primary Care Medical Homes (PCMH) and ACOs and various reporting requirements. PCPs are already seeing increasing appointments and requests from patients wanting nothing more than prescriptions for OTC medications since that’s a new requirement for pre-tax reimbursement using a Flexible Spending Account (FSA)[3].
Looking forward, there is also the possibility that primary care becomes even less attractive to medical students as the practice becomes more constrained with the emergence of narrow practice guidelines (see table below for impact on primary care).
Patient provider choice is another area where we are starting to see corporate moves likely leading to a reduction. Accountable Care Organizations, narrow network products especially those that are provider-managed, will all restrict choice to varying extents. The way this will manifest for consumers of course is that many people will need to change their doctors. This in itself puts an additional burden on the system as new patients tend to need more work-up. Recent examples include the collaboration between Aetna and Carilion and between Tufts and Steward.
Meanwhile, insurance choices are likely to thin out (outside of the exchanges). We’ve seen varying estimates of how many employers will drop coverage and some early evidence of the dropout rate[4]. We have already seen dozens of child-only plans dropped as a result of the guaranteed issue requirement[5]. Many high-deductible plans and limited coverage don’t meet the bar for coverage and will soon no longer be options once the waivers many of them have received run out. Likewise many employers have signaled that they will drop employer sponsored retiree plans as a consequence of the repeal of the Medicare part D pharmacy subsidy.
Some aspects of reform will obviously directly increase cost. Expanding entitlements such as Medicaid (to 133% FPL) and Medicare (closing the donut hole and reducing the catastrophic coverage threshold, extending Medicare to disaster victims) and adding new entitlements such as premium credits, all increase cost in the system. Other effects on cost are not so obvious. For instance, increasing the Medicaid rebate and extending it to Medicare Advantage may reduce price for government but it will likely increase societal costs in other ways such as higher commercial price for new products at launch as the CBO has shown to have happened in the past with Medicaid rebates[6].
Also, in the short to medium term, there is evidence that insurance premiums and cost sharing are rising faster than without reform because while the benefits from prevention and quality improvements take time to filter through, the additional costs to the system for instance from a degradation of the risk pool hit immediately.
There are other indirect ways in which costs in the system are affected. As high risk people are added into the system and everyone’s rates go up, there may be a natural tendency for people to increase their utilization as they argue that they’ve “paid for it so might as well use it”. There may also be some of the “in and out” behavior and adverse selection that Massachusetts has seen as people choose to pay the penalty when healthy and jump on to the exchange in anticipation of health care utilization only to jump back off after the episode of care (the 6-month cool off period in the high risk pool should help reduce this problem though).
Finally, as providers take on bundled payments, there is an incentive to over diagnose patient risk factors at the outset in order to game the bonus mechanism. This will also lead to over treatment though certainly not as egregiously as happens under fee-for-service.
Hospital consolidation, which has been accelerated by health care reform, will also lead to higher prices[7],[8] while many small practices are likely to be forced to merge into larger groups simply because the fixed cost of managing all the complexity of the new regime will overwhelm small practices[9]. While this trend started before health care reform[10]clearly reform provides additional impetus to consolidate.
Another area where reform results in countervailing forces is in transactions costs. On the one hand, the act tries to introduce standardization around data reporting, consumer communication and other areas but it also imposes onerous administrative requirements and increases complexity. For instance, there are multiple new payment models introduced, including various versions of bundled payments and pay for performance and many others being tested. Just keeping up with the paperwork (or electronic work) required to comply with various reporting requirements increases complexity for providers.
Some of the behaviors seen in previous pay-for-performance experiments have also led to the development of arguably counter-productive “innovations” such as “up-coding” and predictive modeling with the sole purpose of cherry picking patients (if a provider is better at predicting risk than the standardized risk categorization used to determine bundled payer, then they can capture “savings” that are not really savings). All of these increase complexity and administrative burden.
With so many of these unintended consequences showing up over this last year and more undoubtedly emerging over time, now is a good time to step back and think about how to anticipate and fix the downstream issues before they overwhelm the intent of reform.
Ironically, while both the left and the right have their own radical alternatives –single payer vs. Medicare vouchers – each of these will have unintended consequences of their own making. These extend well beyond health care, indeed into the realm of revisiting the idea of what it means to be America. That’s another article.
[1] Wall Street Journal, How Health Reform Punishes Work, Daniel Kessler, 4/25/2011
[2]Assn. of American Medical Colleges work force projections
[3] Wall Street Journal, In Health Law, Rx for Trouble, 3/9/2011
[4] Kaiser Family Foundation Employer Health Benefits 2011 Survey
[5] Wall Street Journal, In Health Law, Rx for Trouble, 3/9/2011
[6] CBO Study 1/1996 How the Medicaid Rebate Affects Pricing
[7]Health Affairs Sep. 2011 vol. 30 no. 9 1728-1733
[8]As They Consolidate, Hospitals Get Pricier, Kaiser Health News 9/26/2010
[9] More Doctors Giving Up Private Practices, New York Times, 3/25/2010
[10] Irving Levin Associates, Inc., The Health Care Acquisition Report, Fifteenth Edition