Summary
- Administrative clearinghouse NaviNet has been acquired by 3 Blues plans and a provider of analytics capabilities for plans and providers (Lumeris).
- Both NaviNet and Lumeris appear to need a strategic breakout. The key opportunity is coupling sophisticated cloud-based (=EMR agnostic) analytics with a real time communications platform touching 130K physician offices.
- If viable, cloud approaches to ACO enablement could reduce the upfront infrastructure cost for providers to go at-risk, therefore allowing smaller scale provider groups to participate in the new economics – an attractive proposition for payers unnerved by provider consolidation. But it is a big “if”.
- The Blues investment suggests that the communications platform has become a strategic asset (quite a change from several years when neutral multi-payer portals were the preferred model) — perhaps to support highly differentiated strategies on reimbursement.
* * *
Yesterday, three major Blues plans and Lumeris (an ACO enablement company) acquired NaviNet, an information clearinghouse between payers and providers. Terms were not disclosed though one press report suggested a nine figure valuation. The new ownership is complicated structurally (more on that in a bit) but brings together an interesting mix of capabilities. Also, the potential strategies implicit in the deal provide some clues about where these Blues might be headed in their provider strategy.
NaviNet
NaviNet provides real-time communications platform between providers and payers delivering 50 or so different administrative (e.g. patient eligibility verification, pre-certifications), financial (e.g. claims status) and clinical (e.g. care gaps alert) transactions. About 130K physician offices used the NaviNet Insurer Connect product (though not exclusively). Their revenues were an estimated $55M in 2010 (per Healthcare Informatics) derived from a mix of SaaS and transactions based revenue models. Allowing for some growth revenues and using market cap to revenue benchmarks from public comps (around 2.5x) suggests an overall valuation of about $150M (consistent with the publicly disclosed data point).
NaviNet competes vs. a range of clearinghouse players such as Availity, Instamed, Emdeon, or HealthFusion (see here for Aetna’s list of partners). Yet, as the costs to connect have been going down, the standalone clearinghouse model seems less and less defensible. As a result, in 2010 NaviNet started trying to get closer to the provider by launching practice management and EMR products (sold under the positioning of UPIM – Unified Patient Information Management) as well as the acquisition of Prematics for mobile messaging. It does not seem like these efforts have gotten much traction, however: as of 9/11, NaviNet had only signed up 1K docs for the PM and EMR systems. But it’s a crowded path they are marching down: Emdeon has their Clinician EMR and Athenahealth has its Clinicals – not to mention all the other EMR vendors out there.
Essence and Lumeris
Essence is a Medicare Advantage plan with about 40K lives mostly in Missouri, Washington, and Illinois. It is privately backed (Kleiner, Perkins Caufield and Byers) and operates with a heavy primary care orientation (for example: smaller panels, bigger rewards including – per releases – PCP incomes 2x the national average, benefits design with low cost sharing for routine physician visits, heavier cost sharing for hospital). It has achieved 4+ star ratings across its plans, although it has had some trouble expanding to new geographies (for example, after entering in 2008, it exited Kentucky and Indiana markets for 2011 leaving 9K members behind).
Lumeris is a fully-owned subsidiary of Essence and has been productizing (under the Maestro and Tacklebox marks) the various cloud based analytics software tools developed to support the Essence health plan and doctors. If the health plan is a bit of an also-ran (membership down 20%+ in 2011 due to KY, IN exits and sharp decline in WA membership), smart money seems to think that the tools which support the outcomes have real potential and investment has been flowing in ($70M in 2011 targeted for Lumeris).
So far, however, the commercialization seems modest: Lumeris claims as customers 18 physicians groups, Blue Cross Blue Shield Florida, Network Health Plan in Wisconsin, and WellMed in Texas. The provider groups likely overlap with Essence providers; the BCBSF deal dates from June 2010 and was focused on South Florida Medicare Advantage and sounded per the press release as fairly generic data integration (bringing claims, Rx and labs into data warehouses to make them available for analysis and identifying intervention opportunities); the Network Health Plan deal dates from 4/2011 covers 42K lives. Wellmed is a Texas medical group with 87K patients and which sold its HMO plans to United last year.
The combination
Both NaviNet and Essence / Lumeris appear a bit boxed with their current models. What could the combination bring? A couple thoughts:
- An improved value proposition for the NaviNet EMR by adding a layer of tested ACO enablement analytical capabilities, thereby looking beyond the various Meaningful Use incentives to the more sustainable outcomes incentives.
- A more defensible position for NaviNet in revenue cycle management (RCM) vs. the major EMR vendors by having Lumeris cloud and API interfaces sitting between any installed EMR and the NaviNet software.
- Cloud based ACO enablement tools integrated into the real-time administrative transaction flow: get real-time care plans for each patient which will maximize performance vs. the quality and cost targets in the payer contract and optimized vs. the data the payer sees through the transactions. Particularly if the public health information exchanges are slow or end up being trumped by private HIEs in select markets (as may be happening in the Pittsburgh area), integration of the claims data into the clinical ACO enablement will be valuable. I think also this may represent an advantage vs. United’s cloud offering.
- A clear signal to the providers in the Pennsylvania/New Jersey markets regarding which clearinghouse (NaviNet) is preferred by the leading local payers, helping to define a standard for providers to build around (particularly if by working with this channel they can more readily access the support tools, data and bonuses associated with going at risk).
Interesting hooks. But there are also risks:
- How valuable is software based enablement of ACOs as a stand-alone? One can argue that ACO formation is 40% change management, 40% care capability enhancements changes and 20% analytical tools. If so, the combined Lumeris/NaviNet model is still incomplete as an enabler.
- How incrementally costly will linking Lumeris’ cloud with the installed base of EMRs be? Lumeris talks about its “tiger teams” for developing custom APIs but that added complexity may be a barrier compared with a single vendor solution (i.e. an EMR vendor which offers integrated analytical tools and an RCM solution).
- Are providers really going to regard ownership of an ACO enablement capability by the local leading plans as a net positive or is the potential risk of becoming too dependent on the strategic objectives of the health plan a net negative?
- By investing in NaviNet, has Lumeris diminished the possibility of working with other clearinghouses such as Availity (owned by other Blues plans)?
- Will Blue plan ownership put any of NaviNet’s legacy payer customer relationships / revenues (e.g. Aetna) in danger?
Net-net, I expect more will have to fall into place for this deal to be successful. Payers eager to enhance the performance of independent providers (e.g. Highmark in its competitive struggle vs. UPMC) have a lot of reason, however, to make this successful.
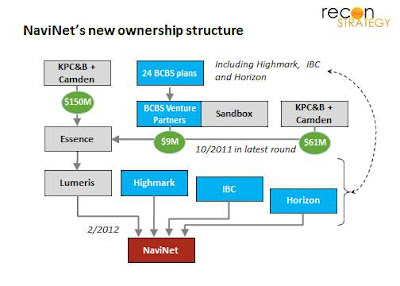
A few thoughts on the new ownership structure which seems complicated:
The Blues system (through its BCBS Venture Partners arm) has a small share of Lumeris’ parent firm Essence (maybe a 2% share based on some back of the envelopes). The three investors in NaviNet (Highmark, IBC and New Jersey) participate in the BCBS Venture Partners fund but their share is obviously indirect and highly diluted.
At the same time, the three Blues plans participated directly on the NaviNet acquisition. While the shares not are disclosed, the funding might well be non-trivial. If Lumeris invested all the $70M it raised in 2011 in NaviNet and if NaviNet was valued at only $100M (minimum given the public statement of a nine figure value), that still leaves the Blues plan owning 30% of the company.
Why the complexity? This ownership structure hints that the Blues be hedging their bets. They did not, after all, choose invest at the level of Lumeris (and thereby own indirectly NaviNet) but at the NaviNet level. On the one hand, if Lumeris / cloud-based ACO enablement takes off, they control the connectivity. On the other hand, if it does not succeed, the physician connectivity is not stranded in a struggling company. As always for the Blues: the provider relationship is to be jealously guarded.