- Employer adopts a tightly limited provider network
- Customers sign on to private exchange
- Hospital chain grows through acquisition
- Insurers boycott state exchange
- Health systems drop out of ACOs
- Payer collaborates with provider systems to target Medicaid population
All of these represent choices or “bets” that firms are making based on a view of a healthcare world facing clear trends.
- More people have health coverage
- Consumers have more “skin in the game” and are more engaged in making healthcare choices
- Providers are paid for performance, not transactions
- Employers are increasingly cost conscious
Now, there is no doubt in anyone’s mind that these trends are real and that they need to be considered as payers and providers develop their strategy. But developing strategy around these trends is not sufficient because there is a much more fundamental uncertainty around how the industry will evolve and that’s what will ultimately determine the pay-offs and winners and losers in this game. And there will be more losers than winners.
We outline two scenarios that arise from the very same trends but that have profoundly different implications for strategy. Characteristics of each local market will determine which of these two scenarios will emerge in that specific market.
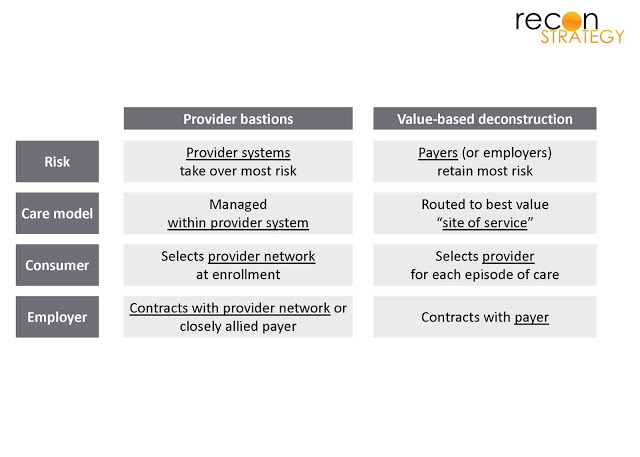
Provider “bastions”
Providers take on a central role in population management. They hold most of the risk through capitation like arrangements with payers and potentially through direct contracting. They manage care through muscular primary care and tight control over secondary and tertiary referrals and care protocols within their owned or contracted networks. Consumers choose their network (or provider within a network) and then get all their care within that network. Payers are relegated to administrative functions and functions such as out-of-network utilization management.
Value-based “deconstruction”
Payers retain most of the risk. They use increased transparency into performance and cost of specific providers to determine those that offer the best value. They then incentivize consumers to select specific sites-of-service. Provider services are commodities.
Selected features of these two scenarios are outlined below.