Summary
- Michael Porter and Thomas Lee have articulated a strategy for fixing healthcare focused on restructuring providers and assessing them based on metrics “that matter to patients”
- The most compelling example they cite of system-wide improvement (vs. anecdote) is the case of IVF where public outcomes reporting demonstrates widespread and consistent performance improvement
- However, the IVF story has several unique features which make it an exception rather than a model for improving healthcare
- System improvement cannot be a matter of supply-side restructuring and outcomes metrics: market forces needs to be brought to bear to demand those improvements. For that you need a market defined around transactions that are medically meaningful but also around which the demand side can be mobilized
- Implementing Porter and Lee’s recommendations alone may create more pockets of change but leave the system overall still limping
Michael Porter and Thomas Lee have offered “The Strategy That Will Fix Healthcare” in the latest issue of HBR. A key part of the Porter and Lee argument is that the right metrics will drive system improvement — provided the supply-side is restructured (e.g. get organized into larger, integrated groups specialized around a particular condition, bundle payments, enhance IT, etc.) David Shaywitz has offered an important perspective that generalized metrics can quickly lose their relevance in the face of patient complexity. I want to focus on another point. Let’s assume we can develop metrics with sustained clinical relevance across patients: How can we ensure that they drive tough decisions on care? In the Porter and Lee article, the mechanisms for what will actually drive better performance remain shadowy (is it empowered consumers? referring physicians? competing providers?): however, the authors cite IVF outcomes improvement as evidence that they exist.
Indeed, IVF is the key supporting example they cite (beyond a selection of brief anecdotes). In the case of IVF, outcomes metrics have been disseminated at the provider level since 1997 by law. The authors show a graph of how outcomes (measured as lives births per embryo transferred) for IVF have improved consistently over time and how the performance band across different subsets of providers (segmented by volume of procedures done) has gotten narrower.
The chart is a compelling story (although Porter and Lee only look cycles using fresh, non-donor eggs in women under 38 which represents under half the cycles being performed). But IVF care has a lot of special features, some of which – especially a mobilized demand side — may have been necessary preconditions for the metrics-driven performance improvement which Porter and Lee promise. Their silence about how the demand side is going to be mobilized to make decisions using their proposed metrics hierarchies is deafening.
What’s special about IVF? Three key features (at least):
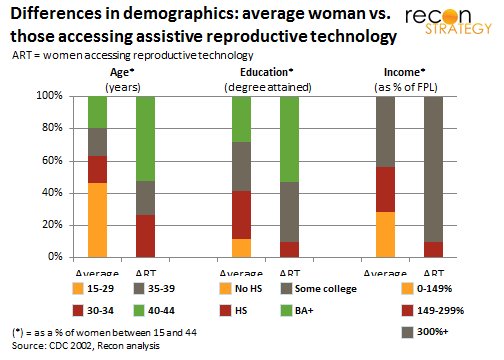
First, a patient population that is older, more educated and richer than most women in the same age band (see exhibit below drawn from 2002 CDC data) and therefore better resourced to make more sophisticated medical decisions.
Second, IVF offers a quickly apparent, relatively binary outcome which is easily measured and patient with a fairly uniform risk profile per age band (women ready for pregnancy) vs. most procedures or physicians where metrics are many and patients with varying comorbidities and risk profiles. This feature forces a sharp focus on the differentials and reduces the potential for physicians telling others (or themselves) that unexplained or unaccounted-for factors drive differences in performance.
Third, IVF offers an actively sought, positive medical outcome vs. other medical procedures focused on the avoidance of a negative or trading off alternative negatives. Prospect theory tells us thatt people frame decisions relative to some reference point and people are bad at assessing low probability negative risks (risks of loss vs. opportunities for gain). Consider, then, the patient assessing relative performance on the key outcome metric for IVF suggested by Porter and Lee (live births per cycle) vs. another patient trying to weigh the proposed hierarchy of metrics for hip replacement such as “pain during treatment” or “risk of complex fraction” or “stiff knee due to unrecognized complications”. It is easy to imagine the first patient coolly reviewing the data and making a rational decision in favor of the best outcomes. It is also easy to imagine the hip surgery patient utterly overwhelmed by alternative bundles of prospective pain offered by different providers under the Porter/Lee model, and see them throw up their hands and say “Doctor, just tell me what I should do.”
The point is not to deny the power of outcomes metrics or the attractiveness of replicating the IVF experience across more medical domains. However, we cannot simplistically extrapolate from IVF (or from the powerful case studies of price reductions in cosmetic surgery) model without carefully considering how and why they worked in this particular medical domain, whether those same conditions apply in other medical domains and if not (mostly the case) whether we can we recreate them. Metrics coupled with restructured provider system will not create a demand side of the market which can drive the kind of creative destruction we need.
Of course, many changes are underway in the provider sphere which will help mobilize the market – among them: changing reimbursement mechanisms, narrow network strategies which drive greater overlap between risk taking providers and insurance, and increasing consumer choice via private exchanges. Integrating the competitive dynamics among these emerging models with clinically meaningful outcomes metrics is critical for the “fixing healthcare”. But Porter and Lee’s proposal is long way from that.
For starters, consider this: We can try to tell patients they should thoughtfully weigh the 20+ outcomes metrics described by Porter, but experts have been telling them to exercise and eat decently for decades and look at how far we have gotten. The healthcare system will need to meet patients more than halfway and communicate value in terms they want and in bundles they will want to assess. To be provocatively ridiculous, how would you rather study your hip doctor’s performance? Relative rate of “regional pain syndrome” or relative rate at which their panels of patients are – thanks to their retruned good health – getting job promotions? achieiving relative hotness? Frequency of fulfilling hanky-panky? Those are some metrics that will get attention! And close study…