Last week, I argued that, if payers want to secure competitive advantage from improved provider care, they would need tighter, more exclusive alignments with these providers to “crowd out” the free riders (the “free riders” in this case are the other payers who have members being treated by the same providers and who can therefore share in any improvements). Two deals last week suggest a case study of the concept may be developing in southeastern Wisconsin:
- On September 9, Anthem announced that it will be teaming up with highly ranked Aurora Healthcare on a narrow network product for the Wisconsin public exchange;
- On September 11, United publicized a major ACO deal with a consortium of delivery systems which compete with Aurora.
A few thoughts on each below.
The Aurora-Anthem deal
Aurora is the largest system in the greater Milwaukee area with 14 acute care hospitals (among them, the #1, #2 and #3 hospitals in Milwaukee per US News and World Report), ~1,500 physicians and reportedly ~40% share in the local market. Aurora has its own ACO platform (branded the Aurora Accountable Care Network or “AACN”) which it sells a number of ways:
- direct (e.g. to the local GE business),
- through Aetna branded as Aetna Whole Health (note: Aetna is pretty much an also-ran in Wisconsin, not even within the top ten),
- through Anthem and branded as Blue Priority (Anthem is the #1 plan with United a very close second).
Since launching for 2013, Aurora claims about 14K lives on its AACN across 40 employer groups (not including Aurora employees which are managed through the same infrastructure). I’d roughly estimate that greater Milwaukee has about 400K commercial group risk lives, which gives the AACN has about a 3%+ market penetration. Modest – but that’s not surprising given that employers had incentives to sit tight with their current plan in 2013 (trend was modest and big changes were certain for 2014 thanks to reform).
The big land grab in 2014 will be on the public Exchange where one recent estimate suggests 376K lives across the state (or roughly 135K in the greater Milwaukee area) will buy coverage. Getting a meaningful share of these lives to overlap across one payer and one provider could nibble around the edges of other payers’ access: if Blue Priority could get 50% of these lives, it could mean a 5-7% boost in Aurora patients. For this reason, Anthem structuring its individual Exchange offering around its Blue Priority network (which is basically the Aurora system in southeastern Wisconsin) is interesting. It suggests Anthem is ready to put its chips down with Aurora and try to crowd other payers out of the Aurora system – even though Aurora (as the premier provider system in the area) is unlikely to be the cheapest system for the price sensitive individual market.
United-QHS deal
How will United (the close #2 in the market) respond? We don’t know the full picture yet since UNH has chosen not to participate on the Wisconsin exchange for 2014. However, last week, UNH announced a major ACO deal with a consortium of Aurora competitors which together have:
- 3,000 physicians,
- 18 hospitals,
- 49% share in the Milwaukee area, and
- 100K United lives.
The participating systems include Froedtert and Wheaton Franciscan (with the #4 and #5 hospitals in the Milwaukee area respectively per US News and World Report rankings). The ACO deal mirrors Medicare in that no member benefit design features will support the ACO structure. The consortium – Quality Health Systems (QHS) – manages the collaboration across participating (and competitive) systems with care coordination support and tools and (presumably) contracting. Apparently, this is United’s first major ACO deal in its home state and appears to be the UNH bet vs. Aurora and Anthem. If the ACO performs, there is every reason to expect UNH to put the QHS consortium at the center of its narrow network benefit designs including an Exchange offering.
Competitive comparison and outlook
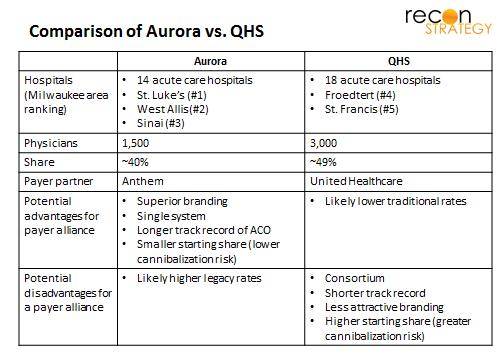
A quick comparison suggests Anthem may have cut the better deal. See exhibit below.
QHS is a consortium with presumably a more laborious governance than Aurora. Its care management capabilities are still nascent (it signed a deal with its care management vendor just this past May). Given that its constituent systems have greater share than Aurora, it has somewhat less to gain from a narrow network benefit design (and therefore less likely to provide strong discounts in return for volume). Potentially the one advantage it offers is a lower set of legacy rates which will lower expectations regarding the upside on any ACO deal, potentially adding to the pricing advantage of a narrow network offering.
QHS may appear the less attractive provider partner, but United may not have an alternative (unless it can pull Aurora out of the Anthem orbit). But, in that case, United does have the advantage of the rich ACO-related capabilities in its Optum subsidiary coupled with a strongly incentivized QHS “shut-out” of the Anthem Blue Priority product. The 3 year term for the arrangement between United and QHS will also allow some time for capability buiids, learning and fine-tuning. Perhaps QHS can make progress fast enough – and be willing to start with rates low enough – to have a real price advantage vs. Blue Priority in 2015.
One side note: United’s cautious approach to the Wisconsin exchange may have tarred QHS a bit. Two hospital systems – Bellin Health Systems in Green Bay and Aspirus of Wausau were originally going to be a part of the QHS collaborative ACO program but backed out in April. Bellin decided to collaborate in stead with Thedacare on its ACO initiative and, interestingly, once month later, Thedacare announced that it would be joining the Anthem Blue Priority network. Will Bellin soon follow Thedacare into the Blue orbit? Aspirus has been part of the Blue Priority network and perhaps its decision to opt out of the QHS ACO reflects a determination that they needed to make a choice and that Blue Priority offered the more attractive path. UNH will need to unwind these decisions or fill these gaps if it is looking for a statewide narrow-network solution.