It is a long-standing hypothesis shared by many providers that community-based interventions that improve primary care could lead to overall healthcare savings by preventing (or delaying) the occurrence of medically expensive conditions. Rigorously proving this has been difficult, and only a few appropriately controlled studies have been published.
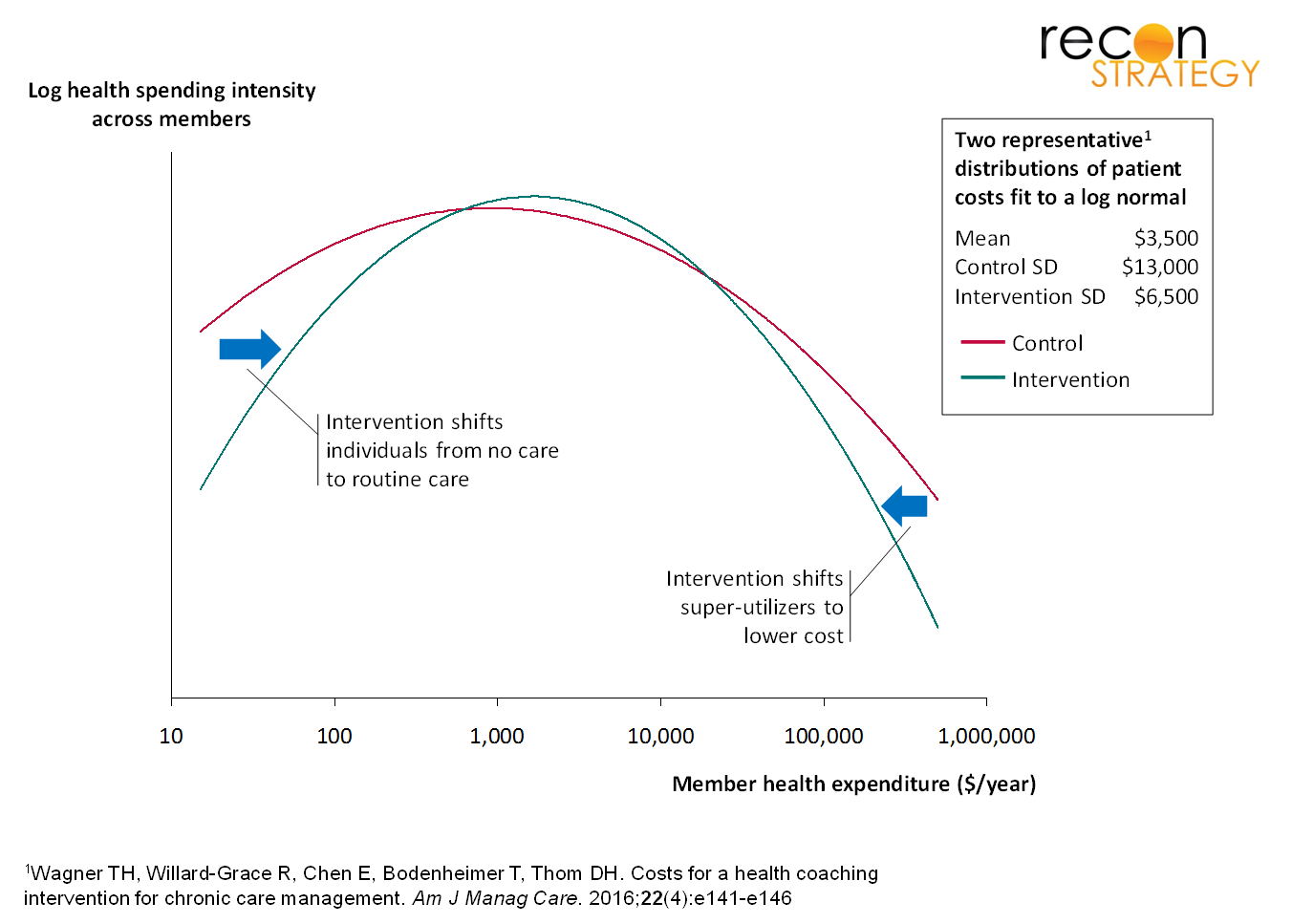
In a Letter to the Editor of the American Journal of Managed Care[1], my colleague Alex Brown and I commented on an earlier article[2] evaluating the impact of a community health worker (CHW) intervention on healthcare costs. The study showed no significant reduction in average cost compared to the control within a year of the intervention. However, we pointed out that it did show a large reduction in the standard deviation of the distribution of individual health care costs (by a factor of 2 from $12,844 to $6,552). This is likely because CHWs promote primary care in individuals who would not otherwise utilize it, and at the same time prevent serious clinical issues from snowballing into medical catastrophes due to neglect and poor follow-up (Figure 1). We then showed that even if the average cost stays the same, decreased volatility of individual health expenditures has economic value to a payer in terms of reducing reserve requirements and/or reinsurance needs. We estimated the value of the study findings using the standard Black-Scholes option pricing of an equivalent financial hedge, and the savings can be substantial (e.g. ~5% of expected cost for small groups).
Figure 1
Although we could not mention them in the limited space of our letter, there are other sources of value that accrue to a health system as a whole from a reduction in the volatility of individual healthcare utilization because the non-cost value of suppressing the long tail of the cost distribution outweighs the increased cost from reducing chronic under-utilizers:
- Significant sudden surges in demand – usually caused by one or two individuals with complex, poorly controlled problems – unpredictably stress the system and tend to decrease quality of care as well as patient and provider experience. Issues range from a waiting time in the clinic that suddenly turns into a couple hours, to lack of individual attention to less acute cases because of the focus on one difficult case, to eventual physician burn out.
- The Lean community has long known[3] that volatility is a driver of waste and inefficiency, and that level-loaded “pull” systems are much more efficient (it is impossible to design an efficient process to produce 5 of something one day and 50 the next). Therefore, less variation in output rate leads to greater ability to optimize the efficiency of a production system. Having to build significant surge capacity in the health system infrastructure for infrequent spikes in demand from under-managed populations is thus intrinsically inefficient. This leads to the existence of mostly idle assets which are a hidden cost that is not usually imputed to the volatility of healthcare utilization, but should be.
A general overarching principle of surgical care is to aim to convert emergency cases to elective ones whenever feasible, because the associated morbidity and mortality is lower. In some ways the same can be said across the health system – the upside from interventions that decrease the volatility of demand is broad, even if they do not result in an immediate decrease in direct care costs. Providers know this instinctively but could make the case more rigorously and forcefully along the lines sketched here.
[1] Herant M, Brown AJ. The value of decreasing health cost volatility. Am J Manag Care. 2016;22(6):448
[2] Wagner TH, Willard-Grace R, Chen E, Bodenheimer T, Thom DH. Costs for a health coaching intervention for chronic care management. Am J Manag Care. 2016;22(4):e141-e146
[3] Ohno, Taiichi. The Toyota Production System. 1978.