About the author: Alyssa Idusuyi is currently a high school senior attending Miss Porter’s School (Connecticut). She spent the summer of 2022 with Recon Strategy as a paid intern assigned a project to research the evolving role of school nurses in student health. Alyssa plans to attend college next year, and is considering a career in healthcare.
School nurses do more than just give students band aids and Tylenol. Since the rise of the COVID-19 pandemic, school nurses have been front and center in taking care of students and faculty. They went from conducting yearly screenings, creating care plans and tracking students with chronic illnesses, completing routine check-ins, and administering medications, to scheduling weekly COVID tests and easing the anxiety within students and faculty regarding vaccines and safety precautions to protect the school community. The increase in attention towards student mental health added to the hefty load that school nurses already have and continue to grapple with. According to the CDC, the percentage of high school students who experienced persistent feelings of sadness or hopelessness from 2009 to 2019 increased from 26% to 37%[1]. Many school nurses feel that, since the pandemic, they have “earned their respect” and are now seen by most as “public health nurses” addressing a broad range of student behavioral and physical health.
How are nurses managing these new responsibilities? In our literature review, we have found that there is little evidence-based work on school nursing practice to guide them. Through our research, we found that school nursing practice in the US is incredibly diverse across states and even inside the same district. Further, most school nurses tend to collaborate alongside two other categories of professionals – school psychologists who help students with behavioral health and school social workers who provide students with the behavioral and social support that they need. However, the amount of access, collaboration, and time that school nurses spend with their school psychologist and school social worker partners varied from school to school and appears to depend on individual comfort and level of experience.
Over the summer of 2022, we interviewed eight school nurses from Illinois, Massachusetts, and Rhode Island. These school nurses came from a wide variety of public schools with different populations and age ranges. There were three topics covered in these conversations — school nurses and their relationships with behavioral health specialists, the role that school nurses play in regards to students getting access to outside healthcare and social resources, and taking a harder look at school nurses managing asthma or other chronic illnesses in students.
Behavioral health is top mind for all school nurses but their approaches can be very different
All of the eight school nurses shared that there is a growing prevalence of issues around student mental health. All the eight school nurses said that in their schools, they are usually the people who identify the behavioral health needs of students and refer them to the behavioral health specialists or better known as the school psychologists when needed. A school nurse who works in Providence, RI shared: “For the most part it’s a clear division of responsibilities. I will refer [the students] over to the school psychologist”. Another Rhode Island nurse who works in a smaller RI community expressed that “we’ve always been at the forefront of finding these students”.
Although each school nurse communicated that there were behavioral health specialists available to the students, the approaches in level of collaboration differed between all of them. While some school nurses said that there was a distinct separation between their work and the school psychologists’, others described their rate of collaboration as more of a “divide and conquer” method. Variety can be found within a single school system: the Chicago school system is wrestling with a nursing shortage requiring that the school nurses in the Chicago Public School district have to work for more than one school at a time, sometimes getting to enter a school just once a week. Perhaps as a result, school social workers seemed to hold a greater presence in some school environments. One nurse said, “CPS is different in that school nurses aren’t seeing students regularly. We’re not based in the building. We’re really only there to take care of kids who have IEPs and 504s who require services… I don’t think our schedules really allow it. I may be at a school once a week but the social worker is there every day.” But other schools in the same Chicago system operate differently: another nurse expressed that she speaks with her school psychologist and social worker almost every day and sets up meetings with the social worker frequently.
School nurses involvement in addressing social needs varies widely
There is similar variation in how responsibilities for addressing social needs are allocated. While some school nurses have had experience with providing students with social needs like giving access to health insurance, other school nurses have rarely addressed social benefits. For the school nurses that do not address the social needs of their students, they usually just refer their students to the social worker to help guide them to external resources.
For example, a school nurse who worked in a school district in Rhode Island communicated that the “social worker absolutely helps to access social resources such as access to local therapists for uninsured students. I don’t touch any of that.” whereas a school nurse in a town school district in Massachusetts shared this: “Usually a bit of divide and conquer. For example, if I’m really busy, I’ll work with one family and they’ll take the next family. It’s very reliant on deep ongoing communication between the two of us”. Another school nurse in Massachusetts, this time working in a suburban school district said “We don’t have a school social worker – sometimes school nurses will actually deliver meals to families on weekends (…) when we need specific social work support, we involve an external social worker.”
School nurses are mostly satisfied with their ability to manage chronic illness like asthma
Throughout the interviews, there were some questions about school nurses and their methods in dealing with chronic illnesses, especially pertaining asthma management. Each nurse unanimously agreed in their interviews that asthma was at least 85-90% well-managed. However, the level of communication that each school nurse had with a pediatrician varied; some talked to a pediatrician frequently whereas others had little to no level of communication with a pediatrician in their time being a nurse.
School nurses support students under a broad range of models
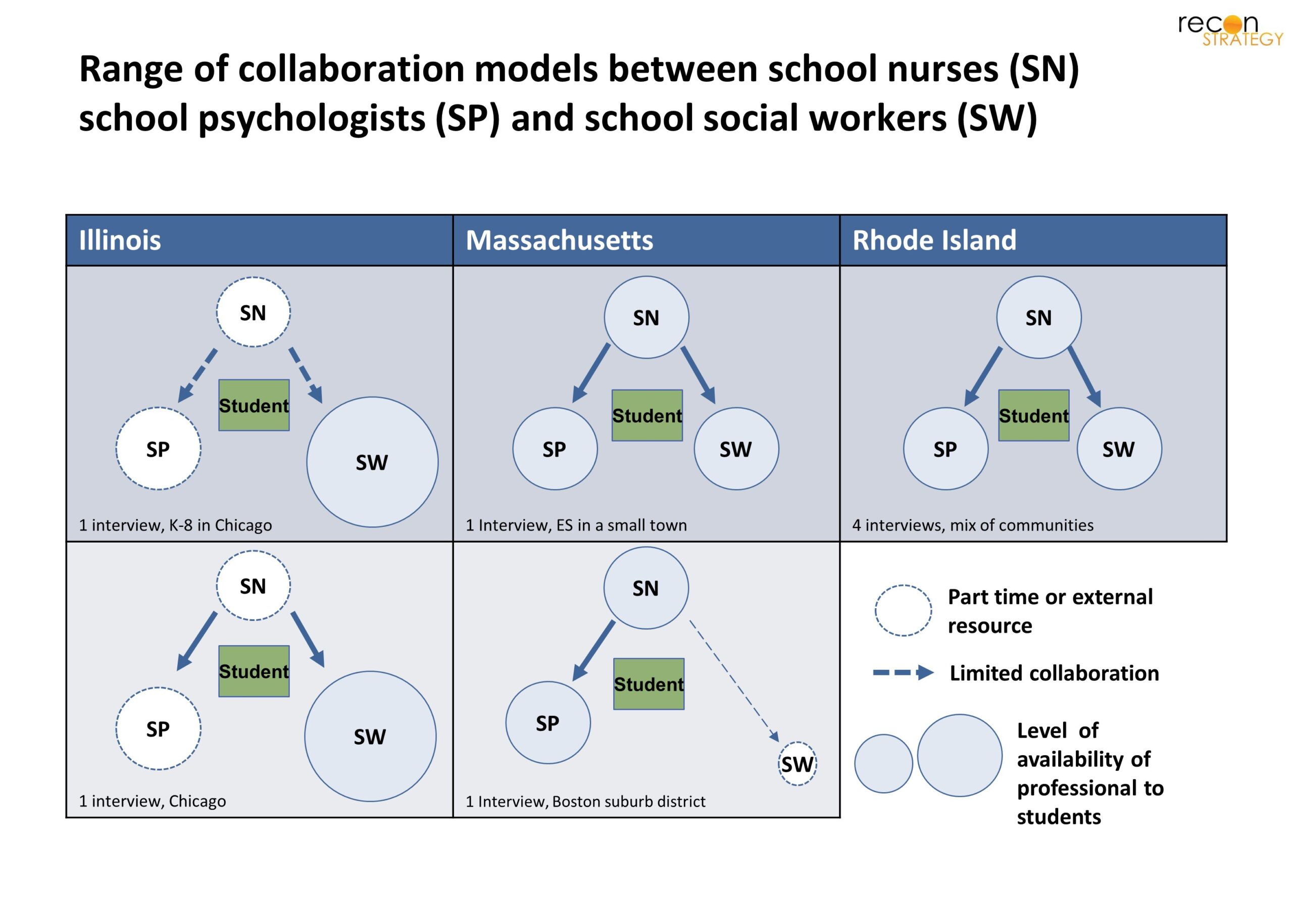
Exhibit 1 displays a high level summary of the different ways the school nurses we interviewed communicate and work with their school psychologist and school social worker colleagues.
Exhibit 1
Across our interviews, there was usually greater consistency of interaction of school nurses with school psychologists. In Massachusetts for example, while the two school nurses we interviewed reported differing reactions level of collaboration with the social workers, they both said that close collaboration with the school psychologist was frequent. The four Rhode Island interviewees all had consistent responses about their collaboration with the school psychologist and the school social worker. Each seemed to work alongside one another at least once a week through continuous check-ins to discuss students’ 504s and IEPs for example.
In the Chicago school system however, the system is clearly different with a large number of school-based social workers and school nurses and school psychologists who each cover several schools.
A state level comparison also indicates a large variation in staffing models
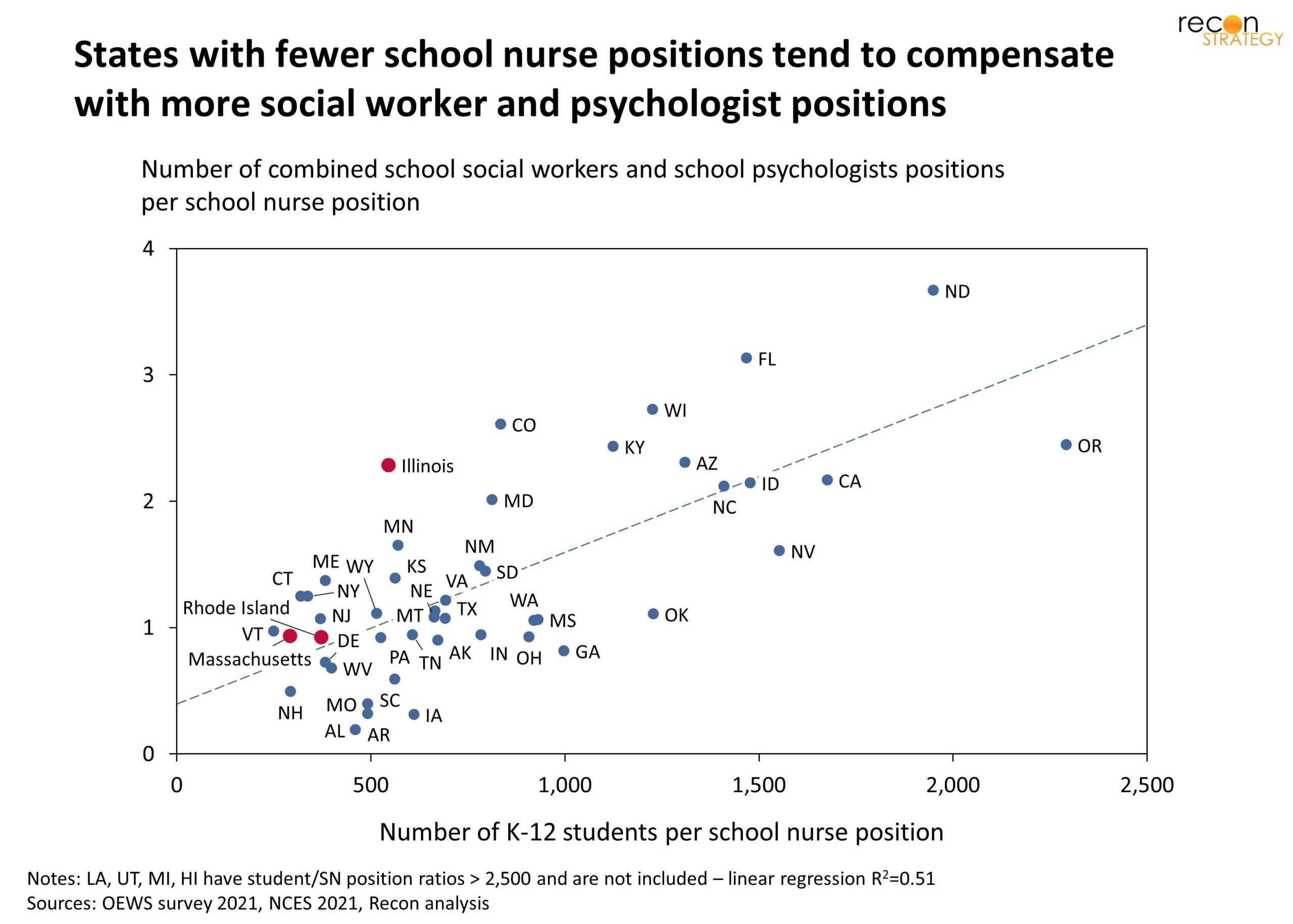
The variability in roles for school nurses, social workers and psychologists we observed from our interviews was matched by variability across states in employment levels per student. We collected quantitative data from the National Center for Education Statistics for K-12 student numbers (Enrollment in public elementary and secondary schools), and from the Bureau of Labor Statistics for a count of school nurse, school psychologist, and school social workers positions by state (for the Occupational Employment and Wage Statistics – OEWS survey, note that a limitation of the OEWS survey is that it counts positions without adjustment for full time versus part time). For each state, we obtained the average number of students per school nurse position, as well as the average number of combined school psychologist and school social worker positions per school nurse position. These are plotted in Exhibit 2.
Exhibit 2
Based on the chart, we still see a wide variation across states in terms of how states choose to allocate their school healthcare resources. In some states, a school nurse position covers many more students than in others. However states seem to compensate areas with a higher student to school nurse ratio by adding more school psychologists and social workers.
Conclusion: a need for research in optimal staffing and working models for school health
There are limitations to our work with a small sample size of interviewees covering only three states and with potential inaccuracies in the OEWS survey (which relies on questionnaires).
But even then it can be concluded that there is no set system in place for school nurses in regards to the extent and type of collaboration that school nurses have with their school psychologist and school social worker colleagues. The level of communication between the three for student behavioral health and social support varies from school to school and individual preference. Interestingly, though, school nurses have definitely stretched their role beyond the physical needs of their students because of the rise in mental health and today’s students need for better emotional support. This raises questions, though: Are the various ways of school nursing practices actually the most optimal ways of doing things? What are some successful methods that have been beneficial for school nurses and their work? Is there even a right way? And for such questions, what we have found is that there is limited research literature or guidelines to turn to.
Likewise staffing levels for school nurses, school psychologists, and school social workers are incredibly diverse across US states and even between districts within states: on the surface it seems that this variation is a result of local decision-making and continuation of past patterns rather than something thought through strategically. In fact, several school nurses we talked to said that if one position could be added, they would rather that it be a school psychologist than another school nurse. While the nurses we talked to did work hard to make the best of what is available to them and were thoroughly dedicated, it is concerning that there isn’t more proactive attention to designing the healthcare support system for students in the face of major increases in mental health and other burdens arising from Covid. More personal accounts and more research is needed in order to better understand optimal strategies that can fully support students and successfully allocate limited resources available to schools.
[1] CDC Youth risk and behavior survey data summary and trends report 2009-2019