Summary
- The case for an oncology ACO can be compelling but CMS rules for ACOs within fee-for-service (FFS) make value difficult to demonstrate
- A new physician-hospital-payer partnership in Florida will test whether the oncology ACO model can succeed outside the CMS rules
- The payer partner has a limited Medicare position and the hospital partner is reputed to be high priced. Despite these potential issues, there are good reasons to think the partners are well aligned on a growth agenda for the model
- If the model itself proves out, however, it may be possible to find applications more broadly (the hospital partner says it is considering cardio ACO next)
Oncology ACOs in Medicare FFS: inadvertent victim of the final ACO rules?
Back in early 2011, US Oncology discussed the idea of creating a national oncology ACO. The key value driver was standardized treatment protocols (Level I Pathways) which a study showed reducing oncology outpatient costs by 35% (focused primarily in chemotherapy and accompanying medications) with no change in outcomes.
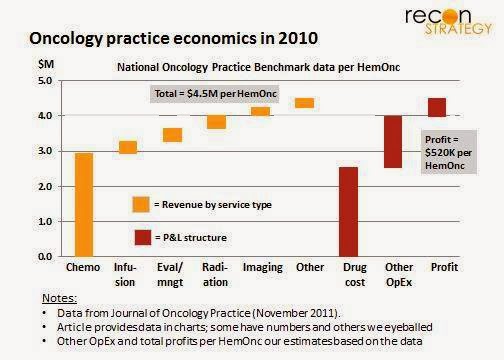
What’s not to love about a 35% reduction for equivalent outcomes? Lower income for the oncologist for one thing. Despite the on-going transition to ASP+6% pricing across many payer contracts, the average practice nationally still earns 65% of revenues from drugs (~$3.0m per oncologist in a community practice) with a reported 13 -14% margin (chemo profit margin = 9% of total practice revenues). Assuming the 35% reduction is in drugs with average margins and no offsetting reduction in fixed costs, Level 1 Pathways could result in a ~$100-150K reduction in gross profits per oncologist. (Data from the Journal of Oncology Practice survey).
However, if payers allowed oncologists to participate in the savings and if some additional cost can be taken out of the oncologist economics (e.g. reduced prior authorization hassle, reduced infusion staffing), oncologists could come out on par or ahead. Incentive alignment with equivalent outcomes! Besides which, there’s a good clinical logic for an oncology specific-ACO: many types of cancers are taking on the characteristics of a chronic condition; further, any comorbidities (e.g. diabetes) need to be managed differently for oncology patients; finally, oncology patients have a unique cost profile and the cost effectiveness of their care might be better evaluated in isolation rather than as part of a broader pool of patients.
Dr. Leonard Kalman, medical director for US Oncology, indicated back in January 2011 that launching a national offering depended on “what is contained in the…final federal rules.” When the final ACO rules were published that November, the oncology community was disappointed. Three key issues:
- The ACO rules compare participating providers vs. historical cost benchmarks yet oncology is an area of rapid innovation (e.g., oncology indications make up a large share of the biopharma pipeline) which typically adds to cost
- None of the quality benchmarks are specific to oncology – making it harder to measure the contribution of excellent oncological care to the ACO bonus
- The most expensive patients are excluded from the cost basis. One estimate puts the cut off at around $100K per patients which is an often used average annual cost estimate of care for someone with cancer. While this feature of the rules removes the penalty for deploying high cost technology (#1 above), it also reduces the ability of the oncologist to contribute to cost effectiveness (if ~half the oncology patient panel is removed from assessment).
Not surprisingly, US Oncology does not have an ACO agreement with CMS and hasn’t been talking much about a national ACO network since.
Can good ideas be saved?
Last month, Florida Blue (formerly BCBSFL), a major hospital system (Baptist Health) and a leading local oncology practice (Advanced Medical Specialties) have agreed to form an oncology ACO in Miami. It is an interesting combination:
- Florida Blue is the largest in the state (4.3 million lives – about 35% of the privately insured lives in the market).
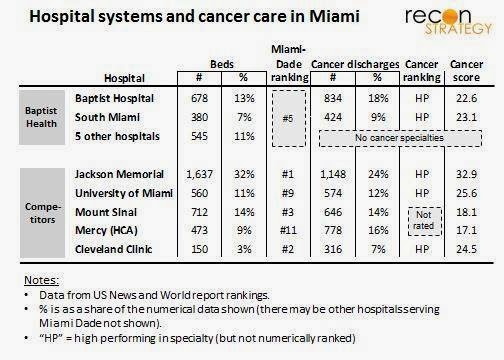
- Baptist Health has 17% of the hospital beds in the market (1.6K beds across 7 hospitals) making it the second largest system behind Jackson Memorial (with 1.7K beds). Also, Baptist has been by far the most financially successful in Miami-Dade and the only one to build a new hospital in 40 years (West Kendall).
- Advanced Medical Specialties (AMS) is a leading practice in Miami Dade currently with 41 oncologists (in a market with 115 active oncologists per Healthgrades.com). It is also an affiliate practice with US Oncology.
There are a few puzzles in this combination:
- Florida Blue’s membership profile is skewed commercial (it has about half the commercial market but very little exposure to Medicare Advantage whose eligibles would benefit the most from cost-advantaged oncology care.
- Baptist Health has a reputation for high prices – 30-40% higher than Jackson according to some. Assuming the data is correct (Baptist’ strong profit margins seem to confirm) and the premiums apply to cancer care, why should Baptist proactively give up the margin. Or, if Baptist is holding firm on its pricing, why should AMS build its ACO with a cost-disadvantage in hospital care (despite historically close ties)?
- Consumers might not regard Baptist Health as an obvious local leader in cancer care. While experts might discount US News and World Report rankings, they do inform consumer thinking – and Baptist competitor Jackson Memorial, University of Miami Hospital and Cleveland Clinic are better ranked (see Cancer score column in table below). What makes Baptist the best partner?
Interestingly, the same Dr. Leonard Kalman who talked about US Oncology’s national ACO strategy back in early 2011 is also the chair of the Board of Managers at AMS and a key architect of the deal. Clearly, disappointment with the CMS rules has not fazed him. Perhaps he is the oncology ACO’s “Gene Kranz” (the “failure is not an option” Houston Flight Director of the Apollo 13 mission) – insisting on fitting a “square” cost effectiveness peg into the “round” hole of the existing delivery system.
Here are a few reasons why this particular combination of ACO partners could work:
Florida Blue’s cancer cost problem
Florida Blue reportedly spends 16% of medical expense on cancer (despite a marginal position in Medicare Advantage) and has been on the receiving end of Baptist Health rates. A custom ACO model could be a clever way to structure a rate reduction win-win outside of the limelight of traditional contracting processes (no financial terms for the ACO were disclosed).
Florida Blue’s small MA position and back-office FFS position
Florida Blue’s minimal Medicare Advantage business in Miami Dade means it has little to lose if the partnership eventually serves other Medicare Advantage plans. In addition, Florida Blue’s position as a Medicare FFS administrator (through is First Coast Service Options subsidiary) could enable it to provide a contemporaneous FFS cost benchmark for the ACO (better than the historical cost benchmarks CMS uses given the pace of oncology innovation). Two good reasons for AMS and Baptist to ensconce Florida Blue in the key data analytics role.
Baptist may see its future in volume, not price
Last year, Baptist’s Chief Strategy Officer talked about starting the planning process for a “world-class comprehensive cancer care center” to be up and active within 3 years. The ACO model can help lock in referrals from a very prominent local practice. Also, Baptist pricing differentials may not be sustainable: Jackson Memorial’s financial position is very weak (there has been talk of bankruptcy after last couple years) but – at 30% of the bed capacity – is too big to fail. In whatever way the financial difficulties get resolved, (and some see solutions in “tapping Baptist Health reserves” cost effective care will likely be critical for the future. Perhaps that is why Baptist has also been talking about expanding the condition-specific model to other diseases (e.g. cardiac care) reinforcing the idea that cost-effectiveness will be a prerequisite for growth in Miami-Dade. Lastly, keep in mind also that the Level I Pathways saved money by reducing chemotherapy costs with equivalent outcomes, not by reducing hospitalizations. That’s different from the stereotypical ACO model of savings and therefore making the oncology ACO perhaps more attractive to Baptist.
Several possible quids for AMS to partner with Baptist
Baptist’s planned state of the art facility should help mitigate any perceived lead Jackson Memorial has in cancer care in the consumer mind. For AMS, therefore, securing access to a new state of the art facility at Baptist may be very attractive. Jackson Memorial has a comprehensive cancer center (Sylvester) but is was built in 1992 and Jackson’s economics may limit its ability to upgrade the facility to match what Baptist is planning. Further, bringing together a hospital with a major oncology practice may create operating cost synergies in the drug management or infusion delivery. Lastly, for US Oncology, striking this deal helps broadening the footprint of the Level I Pathways to the Blues system. After all, Aetna — the payer partner in the original study showing cost savings to Pathways – has dealings with P4, the Amerisource competitor to Pathways.
* * *
ACOs are experimental enough, so it is not a surprise that a condition-specific ACO would require a multi-pronged logic for a first formal test run. And it won’t be easy even if the partnership is solid. Early results from rolling out the Pathways methodology in Texas have been yielding 5-10% savings – not the 35% the original study suggested (admittedly early results off a small base of patients). If it delivers a model for 35% cost reduction while delivering consistent quality and patient-centered care (in this case: treating all conditions appropriately given the oncology diagnosis), who cares what logic led us to it?
(Note: co-written by Tory Wolff and Jamie Matheson with input from Jay Chyung)