Last month, word got out that Verily is in talks with health plans to “jointly bid” on care management contracts. Medicaid populations might be a reasonable surmised as the target given that (1) managed Medicaid requires bidding, (2) Medicaid contracts typically come in packets of hundreds of thousands of lives (which was the scale mentioned in the press reports) and (3) Verily had been considering (but decided against) bidding on Medicaid contracts using Oscar Health as a partner.
It is curious, however, to see an organization seek collaboration with health plan incumbents when its partnered venture arms have invested in three start-ups – Oscar, Clover and Collective Health — to fundamentally disrupt health benefits one way or another (usually by promising a more sophisticated application of technology). A successfully collaboration would, after all, give the health plan partner a deep understanding of what Google has up its sleeve, enabling corresponding capability enhancement and generating equity value for the health insurance partner. Why not keep those insights “in-house”?
It could be that Google is taking a portfolio view and will collaborate with one hand while seeking to supplant with the other. Alternatively, given the disappointing experience of Google’s health insurance disrupters to date, the new partnership strategy likely reflects learnings about how challenging health insurance in fact can be. Let’s take a look at each of the three in turn, then offer some hypotheses about what Google may have learned.
Oscar Health
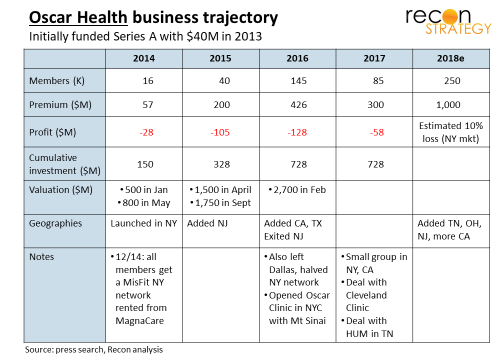
Oscar Health started in 2013 with the ambition to use technology, non-traditional benefits (e.g., no co-pay for primary care, routine care, and generic drugs) and design simplicity to appeal to younger consumers on the ACA exchanges. Google came relatively late to Oscar but committed significantly: it was lead in post-Series C venture round in 2015 and participated in a later private equity round led by Fidelity in 2016.
Google invested during the initial growth spurt: Oscar grew from 16 to 40K members in 2015, expanded in NJ, followed by TX and CA for a total of 145K lives in 2016. But it got into trouble in NY with an expensive rental network from MagnaCare (press reports suggest 30% higher prices than other insurers paid) and “market instability” elsewhere. It abandoned NJ and Dallas shortly after entering and halved its New York network (focusing in on Mount Sinai). Its membership in 2017 was less than 60% (85K) what it was the previous year.
Since retrenchment, Oscar has started to look a lot more like traditional health plan:
- Diversified into small group (contrary to Oscar’s initial strategic perspective that employer based insurance is obsolete), thereby mitigating some of the risk selection/adjustment issues of the exchange and accessing lives with greater average retention which should give Oscar’s technology and value investments more time to pay off
- Made narrow network provider partnerships core to its product strategy (notably Cleveland Clinic in Ohio and Mount Sinai in NY) which has more of the tone of “we know better” rather than “we empower consumers.”
These strategic learnings and reorientation have not come cheaply: Oscar lost a cumulative $300M since founding and expect to run a 10% loss in 2018 (at least for its core New York market). Oscar may still be a unicorn but the valuation last done in February 2016 when the need for a major business restructuring was likely not seen.
Clover Health
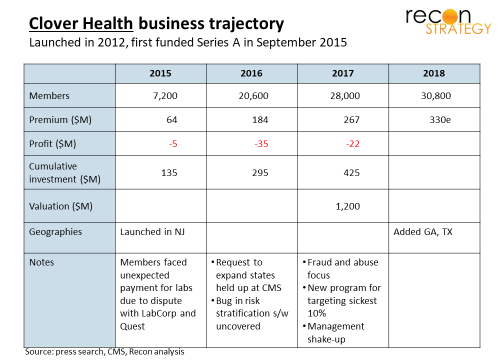
Clover Health is a Medicare Advantage plan seeking advantage by the clever use of technology. Similar to Oscar, Google came in late but, in contrast, the commitment level seems lighter (only participating in one round- the most recent D round in 2017 when the company was valued at $1.2B).
The two lead entrepreneurs were a hospital executive who turned around Carepoint (a small system in Hudson County, NJ) and a technology engineer from a social networking company (Yammer acquired by MSFT). The lack of health plan chops in the leadership showed. Early reports of 50% fewer hospitalizations vs. other Medicare members in New Jersey probably had more to do with heavy reliance on Carepoint as a key provider than any Clover processes (most of Clover’s initial members were concentrated in Hudson county).
At the same time, Clover struggled with:
- Ancillary service providers (Clover held back payments to labs to get access to data, but the labs just billed patients directly creating confusion and complaint in the membership)
- Quality issues (Clover saw a reduction in stars ratings from 3.5 to 3.0)
- Marketing problems (CMS objected to language regarding out of network providers and eventually held up requests to expand to more states)
- Technology bugs (risk stratification software bugs led care managers to call the wrong patients).
Eventually, there were leadership changes and, similar to Oscar, a lot of talking up the adoption of “old school” health plan tactics (e.g., focus on fraud and abuse, targeting the sickest 10% for intervention). Meanwhile, growth has stalled (expansions in GA and TX appear to have added a little over 100 lives) and there have accumulated over $62M in losses (through to 2017).
Collective Health
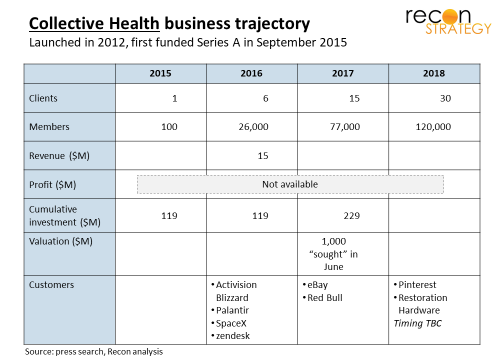
Collective Health is California-based ASO platform touting highly flexible tools, integration of benefit and program choices, and high touch customer and employee services. Google committed early and deeply, participated in the A and D rounds and leading the C round for $81M. Collective Health’s differentiation appears to reside in the real time data and a more personalized level of support (e.g., member advocates, client success managers).
No profitability data has been released but there’s good reason to expect substantial losses: Since ASO customers self-insure, Collective has very limited access to risk margin. Further, ASO is also a highly competitive arena especially at the account size Collective Health operates (averaging 4 to 5K members or – assuming 2.2 members per employee – employers with about 2,000 employees with benefits). As a result, typical ASO fees do not allow a lot of room to fund high touch models and building out a new platform while subscale. The network Collective Health rents (reportedly from Blue Shield of California) is unlikely to be cheap. While it was reported that Collective Health sought more money in 2017 at a $1B valuation, it is perhaps telling that the actual number was not reported.
Still, in the past year, it grew 55% to 120K members which is impressive. But not market-shifting. If it could sustain that rate, it will take Collective Health another 5 years to reach 1M lives. But sustaining the rate may be difficult: it must have helped juice the revenues that several initial account wins were publicized clients have ties to Collective Health’s investors. The identified customers to date certainly suggest a segmented appeal (tending towards technology and self-consciously quirky).
Potential lessons
Each investment covered a different and growing part of the benefits management market – exchanges, Medicare Advantage and ASO, a fact which gives the appearance of a carefully constructed portfolio designed to yield learnings. We don’t know what lessons actually drew, but here are the ones we might have drawn on their behalf:
- Scale is essential. The health plan is the orchestrating and financing component in healthcare, but providers are more essential to driving outcomes and managing costs. Being able to command provider attention by scale in unfragmented blocks of business (avoiding intermediary rental networks) or strategy (narrow networks) is a prerequisite for a health plan to achieve a state of the art outcome
- Scale is hard to come by. Organic growth is safely measured in hundreds of thousands of lives only when you already measure your book in millions. If you grow too fast, you are likely heading for problems (Oscar’s experience in 2016)
- There is plenty of technology in health insurance already. Clever deployment of specific technologies to address specific problems may yield significant benefits, but the impact is easy to overestimate (e.g. assuming adoption rates you see in other industries) and if, along the way, you are also building your own versions of standard systems and processes (like risk stratification), you can get things wrong
- The real impact (and therefore real money) is in risk management not benefits administration. While ASO models (such as Collective Health) may have a less twisted path to profitability than at-risk ventures like Oscar and Clover, they also have less impact on care management strategy because they must administer what the employer wants to put in place
- Insurance’s regulatory complexity can trip up many and executive teams can burn millions learning some basics or failing to mitigate regulatory risks. Experience can help (no wonder Verily has launched a search for a health plan executive!)
If these are reasonable conclusions, then Verily in negotiations with health plans to partner on its big foray into care management (rather than trying on its own) makes more sense. A partner can provide the network, fill in with state of the art capabilities where Verily does not have specific solutions in mind, and have the regulatory approvals and chops to take a significant role in risk.
The question remains: why would a health plan partner which has all these capabilities sign up for a joint venture with Verily? Just what is up that sleeve?